Chronic sleep disorders affect over 70 million people in the United States alone, with Obstructive Sleep Apnea (OSA) accounting for more than 30 million of these cases. Unfortunately, a majority of people with sleep apnea can’t get treatment because they haven’t been diagnosed. According to the American Medical Association, only 6 million Americans have been diagnosed, leaving 24 million on their own. And most people aren’t being screened for sleep disorders.
So why are so many people going undiagnosed?
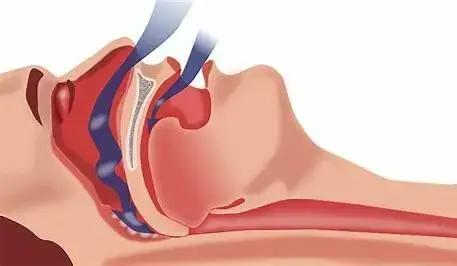
Obstructive Sleep Apnea is a serious health condition and also the most common sleep disorder. People living with OSA stop breathing throughout the night when they’re sleeping due to their throat muscles relaxing to the point of obstructing the airway.
Not being able to breathe through the night is one of the more obvious consequences of OSA, as is snoring, but there are other ways OSA patients’ health is put at risk. OSA patients repeatedly wake up during the night due to a lack of oxygen, but they are not always aware this is happening. This means that during the day, the patient is not rested and feels fatigued – which can be disastrous if driving or working with heavy machinery, but also impacts their overall quality of life.
If a person is living with sleep apnea, they are also at risk of developing other health conditions including high blood pressure, decreased libido, and cardiovascular problems. So, despite what many believe about OSA, sleep apnea is more than just ‘loud snoring’— it’s a condition that can drastically affect a life if left untreated.
What causes sleep apnea?
Several risk factors can contribute to the development of sleep apnea including excess body weight, diabetes, smoking, asthma, sex at birth, and family history. Keep in mind, anyone can develop sleep apnea, but these are some of the things doctors tend to look out for.
Understanding the OSA Patient Population
One of the reasons people tend to fall through the gaps and go undiagnosed is that doctors might have a preconceived notion of what the ‘standard’ sleep apnea patient looks like, and may not detect it in someone who they consider to be a healthy individual. Some of the risk factors we mentioned earlier that tend to get more attention than others are sex at birth, body weight, and the presence of diabetes.
While an older, overweight man may seem like the standard patient, this may not always be the case and is one of the reasons the diagnosis rate is so low. Women can also develop sleep apnea, but are seldom diagnosed. During their routine healthcare visits, they may not receive proper screening, and if they bring up their sleep problems, another sleep disorder may be incorrectly diagnosed, or their symptoms may be attributed to a comorbid condition.
Women’s OSA symptoms can present differently than men. For one, the classic telltale sign of OSA, snoring, isn’t as prominent in women and neither is the lack of breathing during sleep. Fatigue is one symptom that remains constant for both men and women, but for women, it can often be misattributed to a different condition, such as insomnia.
As a healthcare provider, it’s important to screen all patients for sleep disorders, even those who may not appear to have OSA, as it can also affect them during any potential surgical treatment. For instance, when under anesthetic, a sleep apnea patient’s throat muscles may relax and cause the airway to constrict and prevent breathing.
How dentists can treat sleep apnea & why you should consider dental sleep medicine
There are two main forms of treatment, CPAP (continuous positive airway pressure) and OAT (oral appliance therapy). Of the two, CPAP is the most common and uses a machine with a mask attached to provide constant airflow to open the airway and allow the patient to breathe more freely and consistently throughout the night. CPAP machines can be loud and bothersome to wear, especially if the patient tends to toss and turn in their sleep.
The discomfort from a CPAP machine can lead patients to stop using their device – the abandonment rate for CPAP machines is as high as 60%. So, while treatment has been given to many OSA patients, not all of them will adhere to them the way they should.
As a dentist, you’re in a unique position to help OSA patients by delivering oral appliance therapy. For some dentists, dental sleep medicine is a great option because it doesn’t take the same toll on the body that working as a general dentist can. Many dentists would prefer more work-life balance.
With a lower overhead to operate a DSM practice (when compared to general dentistry) and the average reimbursement rate of $3000 per appliance, it’s easy to see how the financial aspect of treating OSA would be very attractive. But there’s one more layer to consider as well: with the acceleration of DSO-driven consolidation in the dental space, finding ways of becoming future-proof has so many dentists looking to shortcuts that are simply and unfortunately the pathway to failure.
Dental Sleep Medicine is still a “blue ocean” of potential with far less competition both locally and nationally, unlike the situation that is mounting as we speak.
What is the Mechanism of Action in OAT?
Oral sleep appliances bring the lower jaw forward, opening up the airway to allow the patient to breathe. When a patient opts for OAT, they get fitted for an oral appliance that appears similar to a mouthguard. To do this, the dentist takes impressions of the patient’s bite.
The size and simplicity of the oral appliance may make it far more convenient for patients to use and also allow for portability during travel when compared to CPAP treatments. According to the Journal of Dental Sleep Medicine, a study conducted showed that 93% of their sleep apnea patients adhered to their OAT treatment – a vast improvement from the 40% of CPAP treatment.
What you and your team can do to help undiagnosed sleep apnea patients
Sleep apnea is a serious condition that can affect just about everyone. While it’s helpful to have an idea of what can cause sleep apnea to develop or what pre-existing conditions can put a patient at higher risk for sleep apnea, it’s also important to keep an open mind. Discard the notion that a ‘standard’ sleep apnea patient exists so more people with the condition can get properly diagnosed.
It can also be beneficial to review your screeners and see where you can add additional questions to screen for sleep apnea. When it comes to your patients, your time is very limited. One solution?
The Role of the Dental Hygienist in Treating OSA
Train your hygienist to screen for OSA. They spend the most time with your patients and are the ones asking the questions every visit. There are simple questions about the quality of their health and sleep that can help identify people who may be suffering.
Dental hygienists are in a unique position to screen for sleep apnea, as they have the opportunity to observe patients’ mouths and airways during regular dental check-ups.
Signs of sleep apnea, such as enlarged tonsils, a recessed chin, or a narrow airway, may be visible during a routine dental exam. This is a triple win: the undiagnosed patient gets a new lease on life, your hygienist sees their work creating a greater impact, and you get a new stream of revenue in your practice.
At the International Academy of Sleep (IAOS), we’ve created a program that does just this: trains your hygienist and equips them to become a true dental sleep expert in your practice.
We partnered with Katrina Sanders RDH to create 12 training modules that begin with an overview of airway & sleep medicine management and end with a deep dive into the business side of dental sleep.
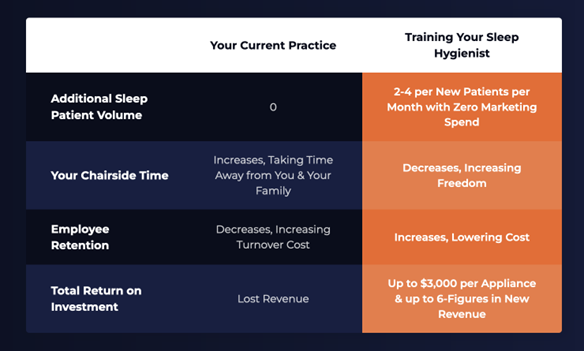
This program easily pays for itself if you think about how much hidden revenue is waiting for you in your hygiene column. In fact, we’ve got a free masterclass showing you real breakdowns of practices and what is possible when you start looking at OSA as an opportunity for growth.