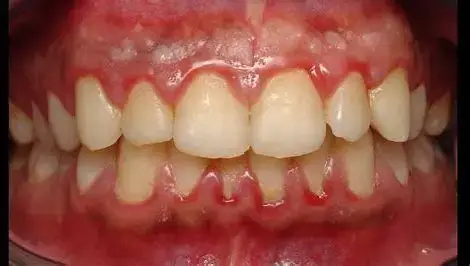
The Greatest Need in Periodontology: A Cure
Periodontitis, termed as the world’s most prevalent infectious disease (Periodontology 2000, Vol. 20, 1999), is much more than a localized oral condition. It stands at the crossroads of oral health and systemic conditions, bearing ramifications beyond what the eye discerns.
The Inflammatory Connection
Chronic inflammation – a silent threat lurking in the background of many major diseases – is gaining prominence in medical discourse, particularly in its association with conditions like diabetes, cardiovascular disease, and even cancer. Indeed, recent insights from Nature Reviews Immunology (2021) suggest that inflammation is the underlying thread connecting these diverse conditions. Positioned at the center of this discussion is periodontitis – the most prevalent chronic infectious disease and a formidable player in systemic inflammatory processes.
Periodontitis and Chronic Systemic Diseases
Americans are alarmingly susceptible to a variety of systemic chronic diseases. From Type II Diabetes and heart disease to Alzheimer’s, the tentacles of periodontitis extend further than one might assume. Here’s what recent studies reveal:
- The Longevity Implications: A 2023 study from J Clin Periodontol, encompassing over 50 years of data from the Veterans Affairs Dental Longitudinal Study, showed that every 1mm increase in alveolar bone loss (ABL) corresponds with a 14% surge in mortality risk. Thus, periodontal health directly correlates with life expectancy.
- Diabetes Link: A longitudinal Swedish study established that a suboptimal response to periodontal treatment (defined by >20% bleeding on probing) portends a 37% elevated risk for future diabetes.
- Cardiovascular Risk: As per IADR 2017, poor response to periodontal treatment (depth of >4mm in >10% sites and ≥20% bleeding on probing after a year of treatment) escalates the risk of heart-related conditions by 28% to 39%.
- Cancer Connection: Periodontal health affects risks of specific cancers. For instance, a 2005 study in the Int J Epidemiol linked tooth loss to a heightened risk of death from upper GI cancer, heart disease, and stroke. Moreover, a 2020 meta-analysis in J Periodontal Res associated periodontal disease with a 40% heightened risk for lung cancer.
Key Takeaways for Primary Care Oral Medicine
- Chronic periodontal infections drastically jeopardize long-term health.
- Effective periodontal therapy is imperative, for subpar results leave patients vulnerable to grave conditions.
- Primary care providers play a pivotal role in preemptively tackling these infections.
The Four P’s of Modern Medicine
Drs. Leroy Hood and Nathan Price, in “The Age of Scientific Wellness” (Harvard University Press, 2023), introduced the Four P’s model – Predict, Prevent, Personalize, and Participate. Applying these principles to periodontology:
- Predict: Gingivitis studies show that clinical signs are not early predictors of bone loss.
- Prevent: Traditional preventative measures, like brushing and flossing, don’t always succeed.
- Personalize: Current treatments may need further personalization for optimal outcomes.
- Participate: Patient involvement is typically limited to education about oral hygiene.
However, introducing saliva testing for periodontal pathogens (Aa, Pg, Tf, & Td) could align periodontal care with the Four P’s model. It aids in:
- Predicting periodontitis during gingivitis,
- Preventing its progression,
- Personalizing treatments, and
- Ensuring patient participation.
Conclusion: Saliva Testing – The Future of Periodontal Medicine
It’s time to recognize the monumental role of saliva as a diagnostic medium for periodontal health. The foundational principles of its application, as outlined in “The Greatest Need in Periodontology is A Cure,” can potentially revolutionize oral care, making it more predictive, preventive, personalized, and participative.
Dental professionals should consider integrating saliva testing into their practices. It not only promises healthier outcomes for patients but also boosts the scope of periodontal offerings.
Action Step: Embrace saliva testing as the panacea for periodontal conditions. Your practice, your hygienist, and most importantly, your patients, stand to gain immensely.